| home > text of the book > section 3> 3.4 |
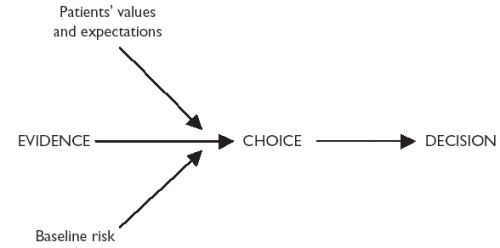
3.4 Skills for decision-making'It is important to distinguish between decision-making and decision-taking' Henry Kissinger Decisions have to be taken on an individual basis because evidence, whether expressed as raw knowledge or in a guideline, has to be related to the condition of the particular patient and their values (Figure 12).
3.4.1 The patient's conditionResearch is done on populations, that is, on groups of patients whose members share a single characteristic, for example having a raised level of blood pressure or having breast cancer. However, these patients also vary from one another in many ways, for example by:
For this reason, information has to be tailored to meet the needs of the individual patient and this is one of the tasks the clinician has to undertake in decision-making. Increasingly, computerised decision support is available to help clinicians and patients relate research findings to individual patients. The National electronic Library for Coronary Heart Disease includes a risk calculator which allows the individual patient's risk factors to be fed into a software system that will produce guidance on their degree of risk. There has been a surge of interest in computerised decision support systems such as Prodigy, but they have not gained wide acceptance, even when demonstrated as being at least as good as clinicians in making decisions. Part of the reason for this is that they are often less good than clinicians, suitably equipped with best current knowledge at the point of decision-making. For this reason, care has to be taken when appraising new computer decision support systems or when reading articles about them. 3.4.2 Patients' values influence their decisionsThe values of the patient have to be taken into account. For example, a patient could be influenced by factors such as the date of birth of their first grandchild, if they are considering intensive chemotherapy with the probability of extending their life expectancy from six months to a year. In such a case, if the chemotherapy appears to give the possibility of surviving to see the grandchild, it might influence them to accept the offer of treatment. 3.4.3 The patient's values and the clinician's values may differWhat is clear is that clinicians and patients have different values, with clinicians giving a higher value to benefit, and patients giving a higher value to the side effects of treatment. One study showed that clinicians would be willing to offer treatment at a level of blood pressure at which only one person in 100 would benefit, whereas patients would accept treatment at a higher level of blood pressure when one in 33 would benefit. This type of treatment decision is particularly important where there are high stakes to play for, for example at the end of life, and Jerome Groopman's clinical enigma (described on pages 55-6 of Second Opinions) illustrates clearly how values can differ between clinician and patient and within one family. 'You all understand the events of last night?' I asked. Before sounding out their wishes I needed to be certain everyone was at the same level of knowledge. 'I think we do', Jared answered. June and Faith silently nodded. Jared continued: 'and we have real concerns about what is happening.' His face was grim. 'What's the point here? Dad has end-stage myelofibrosis. You've got him on a ventilator. He's at a maximum FiO2. His circulation is dependent on a pressor, Levophed. And his creatinine is climbing. Next you'll have to begin dialysis.' I glance at June, then at Faith; each wore an uncertain expression. Carolyn looked perplexed. 'Jared was an ICU nurse,' I explained to Carolyn. 3.4.4 C2P decision-makingThe main mode of decision-making is clinician to patient - C2P decision-making. This usually takes place within the context of the consultation. Although many clinicians, such as radiologists, make decisions which affect patients without these face to face meetings, the final decision is often taken during or after a consultation. Because consultations are very limited in time and are highly charged emotionally, clinicians are increasingly using decision aids to help patients appraise options and consider the decision. These patient decision aids offer patients information independent of the clinician's message and medium. 3.4.4.1 The clinician's messageWhen the clinician transmits information there is always a possibility that:
It is now recognised that the scientific literature on which medicine is based is biased towards a positive and optimistic view of the benefits of medicine for many reasons, such as the desire of journal editors to publish articles with positive findings rather than articles that are inconclusive or negative. Furthermore, it is now known that the way in which many benefits are described in terms of relative risk reduction makes the beneficial effect seem greater than if they were described in terms of the absolute reduction in risk. This phenomenon, which can be observed in clinicians and policy-makers as well as patients, is known as framing. 3.4.4.2 The mediumThe medium, the clinician himself, can be as important as the message, and it is known that the following factors influence the consultation, decision-making, and the eventual decision:
Even the dress and bearing of the clinician can be important, as Jerome Groopman describes in the story (in Second Opinions) about his first-born son. He was strongly influenced by the appearance of the paediatrician, who ... despite the steamy summer heat and the holiday .... wore a starched buttoned-down blue shirt, paisley bowtie and knee-length white coat with his name embroidered in blue script over the left breast pocket. His crisp professional appearance reassured me. In Los Angeles I was disturbed by the indifferent attire of many of the younger doctors: the unkempt hair, running shoes and jeans bordered on sloppiness and did not indicate to the patient the sense of order and attention to detail essential to diagnosis and treatment. The 'professionally' dressed doctor was unfortunately wrong. Face to face communication can be complemented by other media, such as a video. For example, in a study of the use of a video before a consultation in which women were being counselled about the risk of breast cancer, the video was acceptable and beneficial. (3) A systematic review of the research on different methods of giving information to patients with cancer was commissioned by the Department of Health. 120 studies were identified but, using the quality criteria employed in conducting a systematic review, only ten of those studies were considered to provide strong enough evidence to guide policy-makers and clinicians. These high quality studies had examined the effectiveness of:
The researchers found that the interventions had a positive effect on:
The authors' conclusion was that these methods of preparing patients for the consultation, and helping them reflect on it, are 'mostly inexpensive and are not time-consuming to introduce into practice'. (4) Patients can also be given tape recordings of consultations. In a systematic review of eight randomised controlled trials, it was concluded that the provision of written summaries and tape recordings 'helps patients with cancer to remember what was discussed and thus better inform family members'. (5) This practice is now recommended for all consultations about cancer, and for consultations with the parents of seriously ill children. 3.4.5 Patient to patient consultationPatients are also influenced by other patients and this factor is increasingly playing a part in decision-making. Decisions aids now commonly incorporate contributions from patients, and an ambitious project aims to create a database of individual patient experiences (DIPEX) that could be used for education and research and, most important of all, for patients and clinicians to use in decision-making. In Australia, 'peer leaders' of the same age were used in a programme to educate adolescents with asthma. The effects of this programme were compared with the conventional approach, in which education was provided by clinicians. (6) The effects were significant: compared with the clinician-educated group, the peer-educated group had:
Patient to patient support can be very effective. 3.4.6 Clinician to clinician decision-makingClinician to clinician decision-making - second opinions - are part of standard medical practice, particularly when the illness is relatively uncommon, and where the clinician's primary responsibility and treatment options are unclear. Patients sometimes find it difficult to ask for a second opinion. However clinicians, in part to share responsibility, will probably increasingly offer to seek a second opinion, and as medicine becomes more complex and specialised, second opinions will also become more prevalent. 3.4.7 Patient to clinician decision-makingWhat has been described hitherto has been the traditional method of
decision-making, with clinicians initiating and directing the debate.
Increasingly, however, patients are starting to initiate and direct
decision-making and in the remainder of this book we describe how this
approach can be promoted and facilitated. |