| home > text of the book > section 1 > 1.6 |
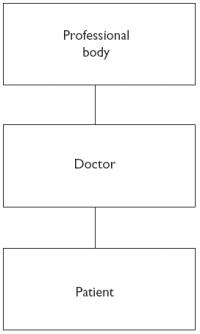
1.6 The decline in bureaucratic authorityBureaucratic power is one of the few types of power held by people, not as a result of their wealth, as in a plutocracy, or their birth, as in an aristocracy, or because of popular mandate, as in a democracy, but because of their position within an organisation. Doctors and other clinicians have had bureaucratic authority to complement their moral, sapiential and charismatic authority. 1.6.1 Professional self-regulation was set up in the 19th centurySarah Gamp, the famous nurse in Martin Chuzzlewit by Charles Dickens, whose sole source of evidence was the imaginary Mrs Harris, could have practised in the United Kingdom until 1902, for it was only then that the Midwives Act was put on the Statute Book, setting up a professional body to regulate them, as the doctors had been regulated earlier by the Medical Act. Doctors had always had some vague accountability, but with the passing of an Act of Parliament doctors were clearly part of a line management system, albeit an imperfect one (Figure 1).
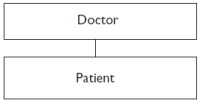
1.6.2 Professional self-regulation fell into disrepute in the 20th centuryGeorge Bernard Shaw called a profession 'a conspiracy upon the public', and the medical profession came in for an excoriating attack in the preface to The Doctor's Dilemma. Although The Doctor's Dilemma focused primarily on the financial drivers of medical decision-making, Shaw also wished to highlight the fact that doctors regarded themselves as accountable to no-one but God, a bureaucratic line with the apparatus of professional regulation being regarded as ineffective in managing clinical innovation or clinical competence. For some doctors, particularly hospital consultants, the criticism was taken even further, and in the year 2000, criticisms of hospital doctors were expressed by saying that hospital consultants considered themselves little gods, i.e. accountable to no-one, as shown in Figure 2.
This situation was unacceptable in the age of consumerism, and two types of bureaucratic controls were introduced: · controls to improve quality and prevent errors; 1.6.3 External regulation has been introduced to supplement self-regulationIn all countries doctors are increasingly held to account as a result
either of court action or a formal complaint. New organisational links
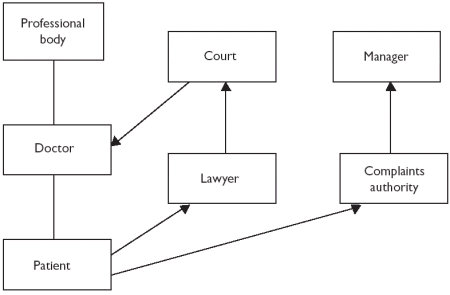
are thus set up between the doctor and organisations other than their
professional body, as shown in Figure 3.
This bureaucratic weight did not increase the authority of doctors. On the contrary, it reduced their authority because patients saw that clinicians had decreased individual power. 1.6.4 External regulation of clinical quality - clinical governance is now in placeIn Figure 3, there is no straight line between the manager and the doctor because the relationship between manager and doctor was unclear. When complaints referred to something to do with the doctor's social
conduct - their politeness, for example, the manager could take action,
but the doctor's clinical performance was left either to the courts
or to the professional bodies to deal with. In 1999, this changed with
the introduction of the concept of clinical governance, which now puts
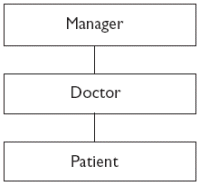
a clear line from the manager to the doctor, covering not only the doctor's
social graces but also their clinical competence (Figure 4).
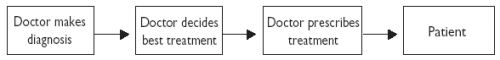
1.6.5 Additional regulation to control costs tightens the screw on professionalsThe fate of Sisyphus was to push a large boulder uphill; even worse, as soon as the boulder reached the top it would roll back down again. Sisyphus or Pegasus(1) is the title of an article in a prominent American medical journal describing the rapid fall from grace of the American medical profession. The image of Pegasus soaring free and unfettered epitomises the American medical profession in its golden days when budgets were booming and a surgeon could simply put up a shingle in a new town and start to ply for trade. As healthcare became increasingly expensive, the middle classes, an important driving force in American healthcare, began to insure against illness, which had become one of the common causes of personal bankruptcy. The insurance companies, who paid for healthcare, were a new force on the American healthcare scene, and insurance companies began to control cost to maximise return for investors as if they were private companies, as many were. In the early days of the doctor as Pegasus, the relationship between patient, doctor, diagnosis and treatment was simple (Figure 5).
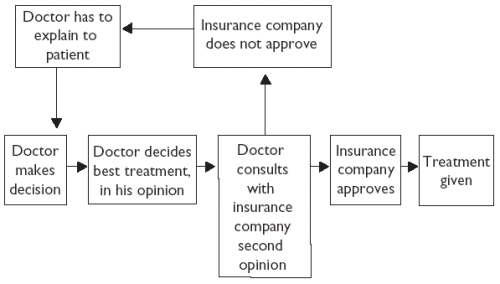
However, diagnostic and treatment guidelines were increasingly introduced, in part by professional bodies keen to reduce the number of court cases and complaints against clinicians, but increasingly by the companies who ultimately paid for treatment. Thus the individual judgement of the doctor was more often tempered by guidelines. Doctors are, however, notoriously difficult to instruct, and compliance with guidelines was shown to be limited. Insurance companies, or health maintenance organisations pressed by insurance companies, began to introduce a compulsory second opinion, illustrated in Figure 6.
With the compulsory second opinion, the doctor seeing the patient had to phone another doctor or, even worse for some clinicians, a nurse employed by the organisation paying for the healthcare, and check through the treatment decision with them. Sometimes a treatment would be refused, and the doctor would have to explain this to the patient. Jerome Groopman describes these conflicts beautifully in his account of his battle with an insurance company in 'The lottery' (in Second Opinions). 1.6.6 Cost control can compromise healthcare providers and cliniciansPartly as a result of the huge payments made to the chief executives
of private insurance companies and health maintenance organisations,
public anger towards these organisations has grown steadily in the United
States, and in the film and book The Rainmaker, by John Grisham, the
insurance company which had refused treatment to a patient on the grounds
of cost, using the excuse of ineffectiveness, was the villain. For some
doctors the imposition by payers of guidelines which could be harmful
to patients has been the last straw, adding to their bureaucratic burden
and reducing their bureaucratic authority (Figure 7).
1.6.7 Declining bureaucratic power, increasing administrative burdenParadoxically, the decline in the bureaucratic power of doctors has been accompanied by an increase in their administrative workload. In 2001, general practitioners in Britain complained about the fact that they often had an hour or two of administrative work every day, much more than was customary a decade earlier, and still had no more clinical time with their patients, whose needs and demands, increasingly more complex and detailed, were being met in consultations which averaged less than ten minutes. It is good that the bureaucratic power of the doctor has been reduced, but it cannot be good that so much of the time that could be spent with patients is consumed by administration. The decline in moral, sapiential, and bureaucratic authority of the
doctor has reduced their status. Now that the doctor is no longer remote
and mysterious, the charismatic authority deriving from that remoteness
and mystery is diminished. |